As its name suggests, post-inflammatory hyperpigmentation occurs following skin injury or inflammation when skin is left darkened and discoloured after the wound has healed. This article looks at how post-inflammatory pigmentation affects skin’s appearance and what causes it. We also identify steps you can take to help reduce the appearance of dark marks on your skin.
What is post-inflammatory hyperpigmentation and what causes it?
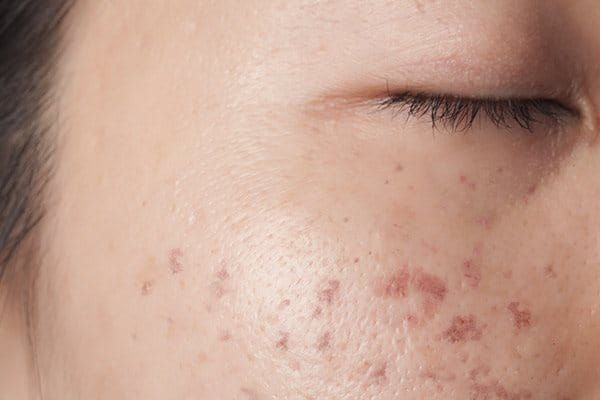
Post-inflammatory hyperpigmentation (or PIH for short) is a type of hyperpigmentation of the skin that is mainly triggered by the way skin regenerates after inflammation. It can affect the face and body, typically especially UV-exposed areas, and appears as flat spots of hypercoloration.
These range in color from pink to red, brown or black, depending on skin tone and the depth of hypercoloration.
Men and women are equally susceptible, and all skin types can get post-inflammatory hyperpigmentation although it is more prevalent in darker tones of skin. In fact PIH is one of the common reasons why people with darker skin tones seek the advise of a dermatologist1.
1- Postinflammatory hyperpigmentation: a review of the epidemiology, clinical features, and treatment options in skin of color. E.C. Davis and V.D. Callender. J Clin Aesthet Dermatol. 2010 Jul; 3(7): 20-31
What are the causes of PIH?
The root cause of PIH is increased melanin production. Melanin is the pigment that defines the color of a person’s skin and the increase in melanin is triggered by the way skin regenerates after inflammation or injury. The more inflammation there is, the more prominent the area of discoloration will be both in terms of size and color.
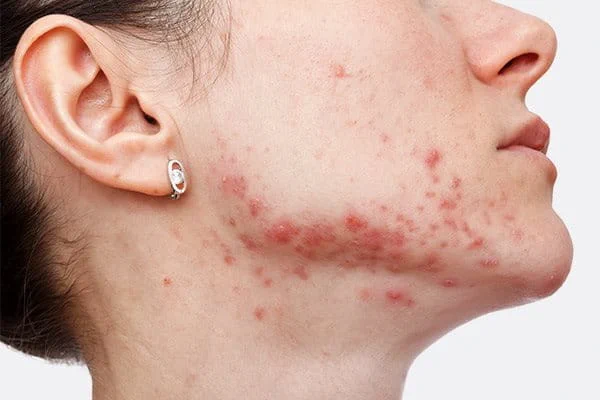

PIH often affects people with acne (also referred to as a post-acne mark) and it can sometimes be triggered by skin treatments such as dermabrasion, chemical peels and laser therapy.
In the case of acne the blemish triggers melanocytes – the melanin-producing cells – to release excessive melanosomes (pigment granules). The excessive pigment granules darken and discolor the formerly stressed area. Once initial blemishes have subsided, spots of hypercoloration, so-called post-acne marks, can remain.
About one in two acne sufferers experience PIH2, with severe impact on their psychological well-being. Studies show that the self-consciousness in social settings or feeling like an “outcast” is significantly amplified when post-inflammatory hyperpigmentation is formed, as compared to acne inflammation alone3.
For many former acne sufferers, the marks are a bitter reminder of their battle with blemishes. Even once the acne-related inflammation subsided, the marks can persist longlasting and stigmatize these patients over years.
2: Source: Kaufman et al., Am J Clin Dermatol. 2018; 19:489–503, Perkins et al., JEADV. 2011; 25(9):1054–1060.
3: Darji, K. et al., “Psychosocial Impact of Postinflammatory Hyperpigmentation in Patients with Acne Vulgaris.” J Clin Aesthet Dermatol. 2017; 10(5):18–23.
The sun is closely associated with other forms of hyperpigmentation such as age spots (also known as sun spots) and melasma. This is why we recommend sun protection. Limit the time you spend in the sun and keep out of the sun during its most intense hours. Wear protective clothing and sun hats whenever possible and apply a sun protection factor of at least 30.
4: Abad-Casintahan, F. et al., “Frequency and Characteristics of Acne-Related Post-Inflammatory Hyperpigmentation.” J Dermatol. 2016; 43:826–828.
Important Information
Post-inflammatory hyperpigmentation is harmless but melanoma can be life-threatening. If you have any concerns about your pigment spots – if they change shape, size and color or if they become itchy and start to bleed – it’s important that you consult your doctor.
What can I do to help prevent dark marks from forming?
If your skin is injured or blemish-prone, or if you suffer from skin conditions such as Atopic Dermatitis or Psoriasis, it’s important that you take care of your skin in order to reduce the chances of post-inflammatory hyperpigmentation.
Appropriate medication and/or a regular skincare routine using products that have been specially formulated to address your skin’s needs will help:
- Atopic skin: you should know how to calm and care for adult atopic skin and best Soothing Care products available in the market.
- Skin undergoing dermatological treatments: you should know what is the best way to care for my skin after laser treatment? And/or what are chemical peels and how do they work?
- Skin affected by minor burns: you should know what’s the best way to care for minor burns?

A sensible attitude to sun protection will also help to prevent or reduce the severity of post-inflammatory hyperpigmentation:
- Limit the time you spend in the sun - Keep out of the sun during its most intense hours
- Wear protective clothing and sunhats whenever possible
- Apply a sun protection product that offers the level of protection your skin needs and that is proven to be suitable for your skin type and/or condition.
Eucerin’s superior sun protection products includes face and body products that are suitable for blemish-prone skin, atopic skin and skin that has recently undergone dermatological treatments.
Does post-inflammatory hyperpigmentation go away?
Post-inflammatory hyperpigmentation does not cause scarring and, even with no treatment, it will improve over time. Most acne-related PIH will eventually fade over time, but it can take several years or even a decade until it is fully gone5. Recovery rates vary from person to person and the duration depends on the difference in skin tone between the natural skin tone and the darkened patches – the more significant the difference, the longer it will take for the tones to rebalance.
5 Abad-Casintahan, F. et al., “Frequency and Characteristics of Acne-Related Post-Inflammatory Hyperpigmentation.” J Dermatol. 2016; 43:826–828.
How can I reduce or remove post-inflammatory hyperpigmentation?
Dermatological treatments such as chemical peels and laser therapy can improve symptoms and speed up recovery time:
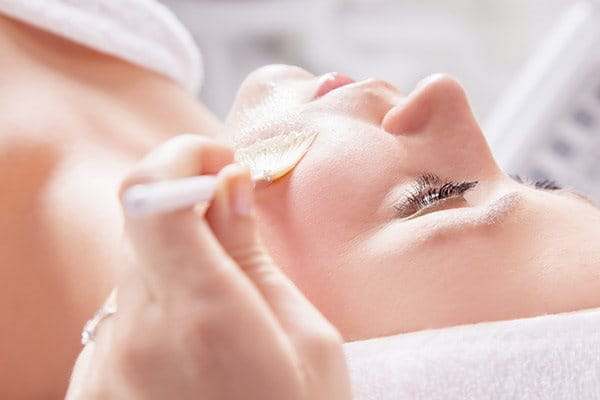
- Chemical peels involve applying a chemical solution (such as an AHA) to exfoliate skin (remove dead skin cells), stimulate the growth of new skin cells and reveal new skin.
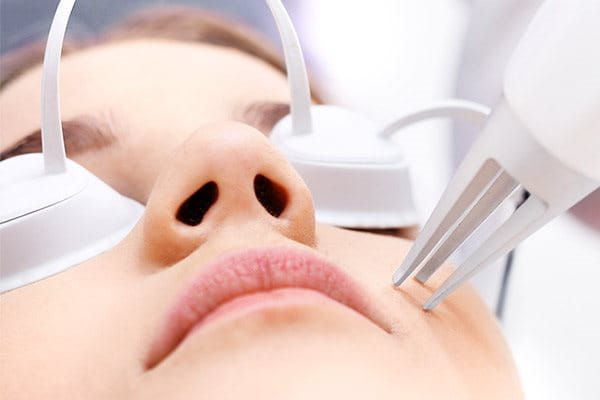
- Laser therapy has a similar effect but tends to be more precise as the dermatologist has more control over the intensity of the treatment. Laser treatments involve ‘zapping’ the affected areas with high-energy light. The mildest treatments work on the skin’s epidermis (surface layer), while more intense treatments can penetrate the deepest layers of the skin.

The Eucerin ProACNE Solution Triple Effect Serum also contain Thiamidol, an effective and patented ingredient that acts at the root cause of hyperpigmentation by reducing melanin production. They’ve been clinically and dermatologically proven to reduce dark marks and prevent their re-appearance.
Our ProACNE Solution Triple Effect Serum combines Thiamidol with Salicylic Acid, Licochalcone A and Sebum Regulating Technology for an effective anti-mark, anti-blemish and anti-shine solution to finally beat post-acne marks. It has enhanced efficacy when used together with the ProACNE Solution Day Bright Mattifying SPF30 which helps protect post-acne marks from darkening due to the SUN.
Our brand values

We deliver a holistic dermo-cosmetic approach to protect your skin, keep it healthy and radiant.

For over 100 years, we have dedicated ourselves to researching and innovating in the field of skin science. We believe in creating active ingredients and soothing formulas with high tolerability that work to help you live your life better each day.







